YOUNGSTOWN, Ohio – Open any job search board and you’ll likely find a plethora of nursing-related positions available.
Exacerbating the shortage of nurses is the lingering demands of the COVID-19 pandemic, an aging population and competition for workers from other fields.
Danielle Bruno, a nursing student at Eastern Gateway Community College, says she can tell that some of her classmates are there only because the field has become more lucrative.
“You just can’t do this job if you don’t care,” Bruno says. “You have to have something in you that wants to help.”
A nontraditional student, Bruno found that her studies at EGCC work well around her job. She believes she was always meant to take care of others and aspires to work in intermediate care, a step-down from intensive care, some day. She worked as an aide at St. Elizabeth’s hospital in Youngstown and fell in love with it.
Her brother is a doctor and her aunt is a nurse, so she has heard stories. She knows it is a difficult field, and she has watched what the nurses she works with go through.
Bruno was working as an aide on a COVID-19 floor during a stretch when fewer than a handful of the patients survived.
“It was awful for all of us, but I think that type of thing built up my unit and the camaraderie between the staff,” she says. “We were one great big family because I spent more time at the hospital than I did at home.”
She feels fortunate because the nurses on her floor are willing to help teach her things, and she knows that the worker shortage means there will be a job waiting for her when she graduates.
Bruno says the shortage is causing a catch-22 situation. It raises stress levels, which causes some nurses to leave the field, making the shortage even worse.
“As an aide, I’ve seen what the nurses go through. It’s very stressful, but sometimes people thrive on stress, and I do,” Bruno says.
Nursing programs in the area are trying to fill the demand as hospitals and medical facilities continue to expand.
Akron Children’s Hospital this month will open a $31 million expansion in Boardman, which will nearly quadruple its previous emergency room space. Salem Regional Medical Center is building a $45 million surgical outpatient pavilion in Columbiana.
Additionally, smaller clinics are being added throughout the region to provide medical options for those in a variety of underserved communities, including rural small towns and inner cities.
“Our growth at this point is very focused on meeting the community where the community is needing,” says John Luellen, CEO of Mercy Health Youngstown, which recently opened a new multifaceted clinic on Belmont Avenue. “Sometimes that need is very transparent, and everybody in the community would see it and agree upon it. Sometimes that need is something we have identified in trends we are seeing through health care operations.”
Although Luellen says they are very cognizant of the labor challenges in the area, he does not believe the system is going to outpace the number of professionals, both nurses and physicians, they can train and hire. Mercy has a 100-year history of providing physician education in the Mahoning Valley through graduate medical education programs. Currently, 150 young physicians are being trained at Mercy, with residencies and fellowships that allow them to further specialize.
Likewise, both Mercy and Akron Children’s Hospital work with the area’s nursing schools and programs to create externships, which are programs where nurses can gain experience on the floor of a hospital.
At one time, nurses had to be in the last year of their program before getting real experience, but not any longer.
Christine Young, chief nursing officer at Akron Children’s Hospital, which employs nearly 400 nurses in the Mahoning Valley, says they adjusted their nurse tech program during the pandemic to allow nursing students in earlier, changing their job responsibilities as their training progresses.
Hospitals and medical facilities are working together to address the nursing shortage. Young notes that Akron Children’s Hospital and the nursing programs at Youngstown State University, Kent State University, the University of Akron and Malone University share an advisory board.
“We talk about the need of the students and the needs of the hospital and how can we better match those and what do students need coming out of school to be successful,” Young
says.
She notes that the pandemic reduced the ability of nursing students to get the clinical experience that once was available, although the situation is improving.
Programs
While the number of students going into nursing has declined nationwide, that is not the case in the Mahoning Valley, says Nancy Wagner, director of nursing at YSU.
The university’s program has grown from 350 five years ago to 800 for both undergraduate and graduate students.
There are already more than the maximum 110 students lined up for the baccalaureate degree nursing program. The decision on who will be accepted will be made after high school seniors receive their grades in May. Many of the students studying nursing at YSU are from the Mahoning Valley, and Wagner says 70% of them remain here after graduating.
That is a good thing, Wagner says, because more nursing students leave the area than come here.
“We truly have to grow our own,” Wagner says. “We feel that obligation in a good way. We know that we need to provide for our community.”
YSU offers two types of nurse practitioner programs: family nurse practitioner and acute care nursing practitioner. Also, there is a nursing education option for the master’s program.
The school also offers a doctorate’s degree for nurse anesthetists.
“We’re really proud of our school. We’re one of largest programs on campus and we just keep growing,” Wagner says.
When students graduate from an area nursing program, they usually have a job waiting for them.
“Right now, the world is their oyster,” says Kathleen Rogers, program administrator for the associate’s degree in nursing program at Eastern Gateway Community College. Local health care providers such as Mercy Health come to the school to recruit workers.
Likewise, Kelly Darney, adult education director at the Columbiana County Career and Technical Center, says for every student graduating from the LPN to RN program, there are 10 jobs waiting for them.
The tech center offers programs in medical assisting, state tested nursing aide and practical nursing.
Like EGCC, CCCTC encourages students to continue moving up the ladder by getting more training and then studying for a bachelor’s degree at Kent State Salem or YSU. High school graduates attending the CCCTC health academy classes can get financial aid if they come back as adults to the nursing program.
The LPN to RN program, which prior to the pandemic had a maximum enrollment of 30 per year, recently graduated 19. Darney also believes the pandemic has had a lot to do with the lower numbers.
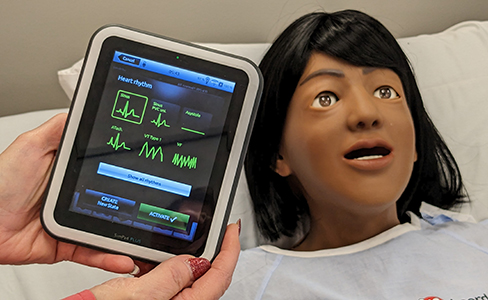
Rogers sees a lot of challenges in getting nursing students to return for more education. But even if it takes 25 years for them to complete their education, she believes letting them work their way through is the best option for many.
She sees programs like EGCC’s associate degree in nursing program as a way out of poverty for many. Students can get their associate’s degree through that program and then go back for their bachelor’s degree later, sometimes with tuition assistance from hospital facilities that are rewarded with a special status for having higher percentages of nurses with bachelor’s degrees.
“What I’m most proud about here is the opportunity to help students who would normally not be able to get an education in nursing,” Rogers says. “Making that happen so they can take care of their families and move up and out, so they can make a better life for their kids.”
The EGCC program graduated 61 in 2021 but is slated to graduate 109 this year. She attributes the rise to the closure of the program at Mercy College.
Rogers says there is also a shortage of nursing instructors. They do not make as much money as nurses, so for one to become an instructor, they would either take a pay cut or continue to nurse while working as an instructor. That leads to fewer able to afford to be a nursing instructor and a nondiverse teaching staff.
“[Students] want to feel like they belong,” Rogers says. “We don’t have diversity in our workforce. We’re all white women. We cannot attract people who are young and can afford to take the cut in pay in order to be here.”
She believes it makes it difficult for nursing students to relate to their teachers, adding that older nurses in hospitals sometimes frighten students away from the profession by being
uncivil to students instead of mentoring them.
She believes teaching nurses to be compassionate with each other and with the patients is an important part of addressing the shortage.
Nurses are leaving because they are burned out.
“We’re a passionate profession, and these people give their heart and soul. They are almost like the unsung heroes,” Rogers says. “Things we do behind the stage that nobody knows we’re really doing, but we are.”
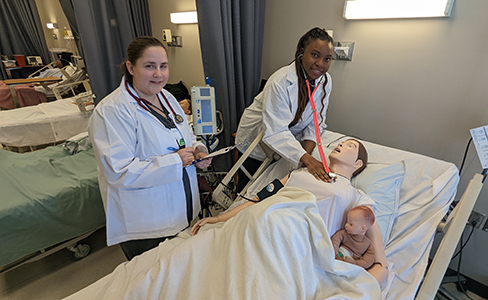
Pictured at top: Eastern Gateway nursing student Danielle Bruno and instructor Kathleen Rogers.
