Improvements in Treatment Help Fight Breast Cancer
YOUNGSTOWN, Ohio – Thanks to improvements in just about every facet of the treatment of breast cancer, those who are diagnosed have greater odds than ever of surviving. Imaging technology is finding tumors early, treatment options are tailored to each patient and resources are available to ease the stress of navigating the health-care system.
“Today, we can diagnose at very early stages. A little more than 90% of cases that we see are early-stage breast cancer, which is thanks to things like mammograms,” says Dr. Roger Hakimian of The Hope Center for Cancer Care in Boardman. “The smaller the tumor, the better the outcome.”
Throughout the region, medical centers have upgraded their imaging technologies – 3D mammograms, ultrasounds and MRIs. For 3D mammography, the technique uses X-rays the same as traditional mammograms but offers a clearer picture to medical staff.
“Instead of looking at pictures, they’re able to look at the entire breast top to bottom and rotate a 3D image,” says Dr. Ayla Kessler, medical director of Salem Regional Medical Center’s cancer center. “It’s advantageous not only to women with cancers, but also benign lesions. It can spare a lot of women from having to come back for biopsies.”
The Salem hospital also has added a new MRI machine that offers double the clarity of previous equipment and is awaiting the installation of a 3D positron emission tomography machine, which can detect metabolic cell changes before anatomical changes arrive.
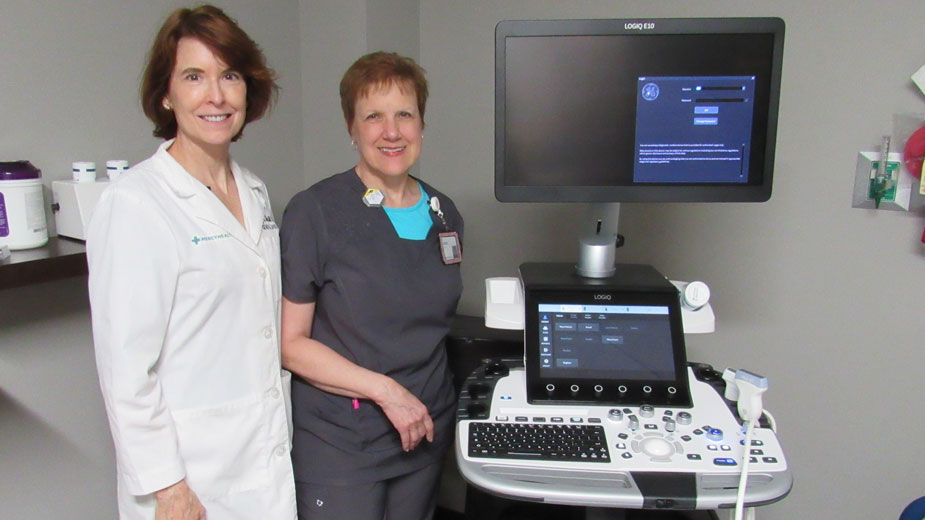
Meanwhile, at the Joanie Abdu Comprehensive Breast Care Center in Youngstown, a new ultrasound machine was installed last month. “We do most of our biopsies with ultrasounds so this is why it’s important we have the absolute best,” says Dr. Nancy Gantt, co-medical director of the Abdu Center. “It’s much more comfortable for a woman to get a biopsy this way where you’re laying down and propped up and super comfortable with pillows and blankets.”
Ultrasound biopsies are also the standard at the Surgical Hospital at Southwoods’ Center for Breast Health, says chief nursing officer Angela Kerns.
“Minimally invasive breast biopsy has become the standard of care,” Kerns says. “We see where we are, we get the markers and then we can tell patients if they need chemotherapy or surgery or a mastectomy. It gives us the opportunity to create an individualistic experience.”
The ability to reduce the number of false starts and enter treatment with a clearer picture is a focus of oncologists throughout the health-care field, adds Dr. Alexis Smith, Gantt’s fellow co-director at the Abdu Center. Even getting called back for a second mammogram adds extra anxiety to an already tense process, not to mention the cost and radiation exposure.
“It used to be with the standard [2D] mammogram images that you had to call back a lot more stuff because you didn’t have these extra pictures,” Smith says. “With [3D mammography] … I can say, ‘No that’s just tissue clumped up,’ or, ‘There’s actually something growing under there.’ ”
After diagnosis, treatments are tailored to individual cases. This often starts with a group of genetic tests of the tumor to determine the risk of cancer returning and how effective hormonal treatment or chemotherapy may be. Even within each test, advancements are coming to provide oncologists better test results.
At the Hope Center, Dr. Amy Awaida points to the Onctotype DX assay, which can help doctors determine how effective chemotherapy will be. The test places patients into three categories: low-risk, high-risk and intermediate. New data out this year has reduced the gray area between high and low risk, allowing doctors to better recommend treatments.
“We didn’t know what to do with those intermediate patients. Do you counsel them to do chemotherapy? Do you counsel them to not do it? How can we reassure them that we’re treating them the correct way?” Awaida says. “Sometimes even early detection may not get you out of chemotherapy. But as we better understand the genetic makeup of cancers, as we understand their behaviors, we can tailor treatment more effectively.”
Such tests can also point to surgery being effective, rather than requiring chemotherapy treatments that can be costly and exhausting, Hakimian adds. By taking the route that is both most effective and less invasive, breast cancer treatment can be less taxing, the doctors agree.

Pictured: Dr. Roger Hakimian of The Hope Center for Cancer Care in Boardman.
“You’re sparing patients the long-term toxicities of therapy. You spare them and society at large the cost of long-term treatment,” says Salem Regional’s Kessler. “Then there are the side effects, some of which are long-standing after patients are done with treatment,” including fatigue, joint and muscle pain and memory issues.
Beyond the medical side of treatment, medical centers are also investing in the personal side of care. The use of patient navigators, who serve as both a guide and advocate, is becoming more common.
“We have relationships with physicians and know [patient] preferences so we can get patients to the next level of care as quickly as possible,” Kerns says. “If you come in for a screening and they see something, we can get you to a diagnostic mammogram and then to a minimally invasive biopsy or an ultrasound. With that navigator, we can get them the most expedited care possible.”
At Southwoods, the time from diagnosis to treatment is seven days, Kerns reports.
A 2017 report from the American Society of Clinical Oncology found the national median time was 29 days in 2013, up from 21 in 2004. Each week’s delay for several types of cancer, including breast cancer, can increase the risk of mortality between 1.2% and 3.2%, the report noted. The five-year average survival rate for breast cancer patients is 90% and the 10-year rate is 83%, the society reported in January. In 1975, survival rate was 65%, according to the Journal of Cancer Policy.
With navigators, patients can move from step to step within the health-care system easier than they could on their own, Kerns says. The duty of helping patients through the process is also necessary on the part of doctors, the Hope Center’s Hakimian adds.
“We can detect them so early that I can tell patients that even if we didn’t detect it this year or next year, the chance of it becoming a problem is small,” he says. “Half of my time is reassuring the patient they’re going to be OK. It always comes with fear. You can go online and see bad information or views. Our job as physicians is reassurance.”
Pictured: Dr. Nancy Gantt, co-medical director of the Joanie Abdu Comprehensive Breast Care Center; and Bobbie Quinn, lead technologist standing next to the new LOGIQ E10 ultrasound machine.
Copyright 2024 The Business Journal, Youngstown, Ohio.