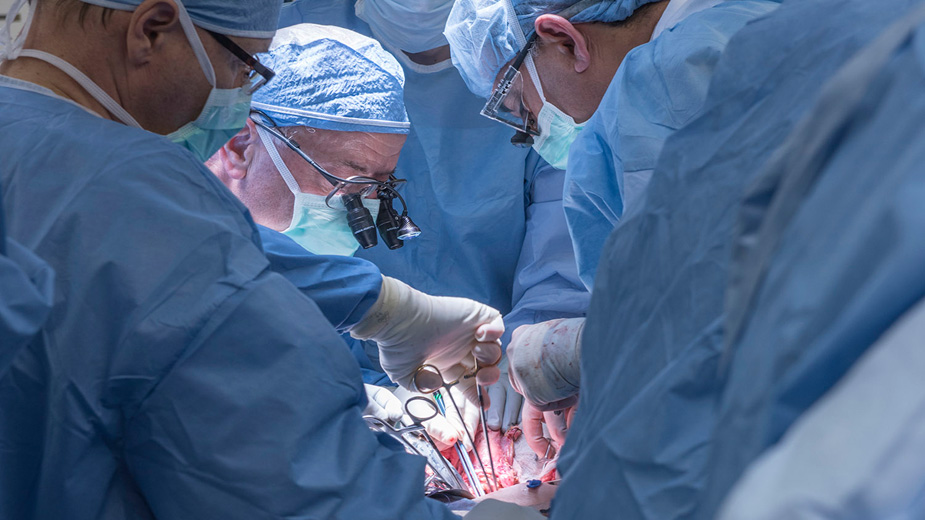
Cleveland Clinic Performs Nation’s First Uterus Transplant
CLEVELAND – A team of Cleveland Clinic transplant surgeons and gynecological surgeons performed the nation’s first uterus transplant during a nine-hour surgery Wednesday.
The 26-year-old patient – who is not being identified publicly – was in stable condition Thursday afternoon, according to an announcement from the Cleveland Clinic. The transplanted uterus came from a deceased organ donor.
Cleveland Clinic will be making no further comments at this time. The surgical team will be available for media questions at a news conference to be scheduled next week
Cleveland Clinic began screening candidates for uterus transplants late last year, as part of a clinical trial approved by Cleveland Clinic’s Institutional Review Board, which reviews and monitors all human-related research projects.
The research team – comprised of transplant specialists, obstetricians and gynecologists, bioethicists, psychiatrists, nurses and social workers – continues to screen transplant candidates with Uterine Factor Infertility (UFI), an irreversible condition effecting 3% to 5% of women worldwide.
Women with UFI cannot carry a pregnancy because they were either born without a uterus or their uterus no longer functions.
The Cleveland Clinic announced in November a new research study in which surgeons would perform uterus transplants in 10 woemn with UFI.
“Although there appears to be potential for treating UFI with uterine transplantation, it is still considered highly experimental,” said Tommaso Falcone, MD, Ob/Gyn & Women’s Health Institute Chair. “Cleveland Clinic has a history of innovation in transplant and reproductive surgery and will explore the feasibility of this approach for women in the United States.”
The first two international attempts at uterus transplant were unsuccessful. Organ rejection during pregnancy was a major factor. After years of pioneering research and human trials (in which Cleveland Clinic took part) a Swedish team was able to manage the mild organ rejection that can occur.
That University of Gothenberg team achieved its first birth in September 2014. To date, the Swedish group has performed nine uterus transplants, achieving five pregnancies and four live births.
“The exciting work from the investigators in Sweden demonstrated that uterine transplantation can result in the successful delivery of healthy infants,” said Cleveland Clinic lead investigator Andreas Tzakis, MD.
Like transplants of the face and extremities, uterus transplant is considered life-enhancing rather than lifesaving, Tzakis continued.
“Unlike any other transplants, they are ‘ephemeral,’” he explained. “They are not intended to last for the duration of the recipient’s life, but will be maintained for only as long as is necessary to produce one or two children.”
Close coordination among the reproductive and transplant surgeons, infertility and IVF specialist Rebecca Flyckt, MD, and high-risk obstetrician Uma Perni, MD, will be crucial to the procedure’s success, the Clinic said in November.
“Study participants will also benefit from the full support of a team of Cleveland Clinic doctors, psychologists, social workers, patient advocates and bioethicists,” noted Dr. Flyckt.
With the green light from its Institutional Review Board, Cleveland Clinic began screening 21-to-39-year-old women with UFI for transplant in September. Each candidate faces extensive rounds of medical and psychological evaluations by experts from different disciplines and must be unanimously approved by the team.
Once a patient is approved for the study, she follows this complex, intricate protocol:
- Her ovaries are stimulated to produce multiple eggs, starting the in vitro fertilization (IVF) process.
- Her eggs are retrieved, fertilized with sperm in a laboratory, and frozen.
- Lifebanc, an organ procurement agency, begins the search for a donor.
- The donor’s next-of-kin signs an informed consent for uterus donation.
- The donor uterus is transplanted within six to eight hours into the patient’s pelvis.
- Over 12 months, the transplanted uterus fully heals.
- One year after transplant, the frozen embryos are then thawed and implanted, one at a time, into the patient until she becomes pregnant.
- During her pregnancy, she takes anti-rejection drugs.
- She is monitored by a high-risk obstetrics team throughout pregnancy and delivery.
- She has a monthly cervical biopsy to check for organ rejection.
- The baby is delivered by cesarean section.
- After one to two babies, she has a hysterectomy to remove the transplanted uterus.
- Her anti-rejection drugs are stopped after hysterectomy to reduce long-term exposure to transplant medications.
SOURCE: Cleveland Clinic
Copyright 2024 The Business Journal, Youngstown, Ohio.